Manhattan's
Award Winning Podiatrist
New York Foot Experts, Provides Specialized & Advanced Care For Your Feet and Ankles
Welcome to New York Foot Experts, Podiatrist Located in Midtown, Wall Street, & Harlem, NYC

New York City’s premier specialists in foot and ankle care. We believe that prompt diagnosis, early intervention, and prevention are essential for the care and treatment of your feet. Dr. Daniel Drapacz and his team specialize in ingrown toenails, bunions, gout, athletes’ foot, foot injuries, ankle injuries, heel pain, plantar fasciitis, and much more.
For more information, call us today or book an appointment online.
We have four convenient locations in NYC:
We serve patients from Midtown NY, Wall Street Financial District NY, Harlem NY, Lower Manhattan NY, Brooklyn NY, and Yorkville NY.
FOOT & ANKLE INJURIES
HEEL PAIN & PLANTAR FASCIITIS
INGROWN TOENAIL
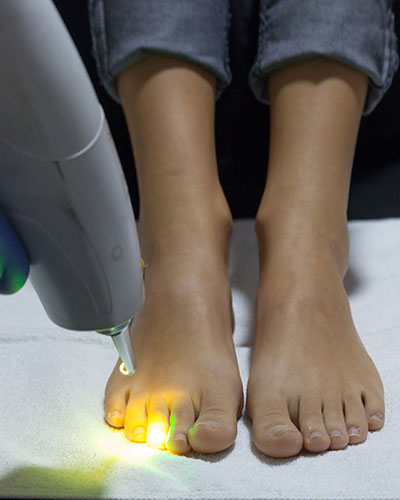
STATE OF THE ART FOOT SOLUTIONS
Dr. Daniel Drapacz, DPM
Board Certified Podiatrist, Foot & Ankle Surgeon
CHIEF OF FOOT & ANKLE SURGERY FOR
TWO AMBULATORY SURGERY CENTERS
Dr. Daniel Drapacz NYC’s Celebrity Foot & Ankle Specialist with over 25 years of experience. Dr. Drapacz specializes in Cosmetic and Reconstructive Surgery of the Foot and Ankle. Dr. Drapacz employs the latest Hi-Tech Laser equipment and advanced surgical techniques to achieve superb results for his patients.
PATIENT
REVIEWS
"Excellent service, friendly staff"
NEW PATIENT
OFFERS
TAKE ADVANTAGE TODAY!
SCHEDULE AN
APPOINTMENT
We will call you to confirm your appointment.
PATIENT REVIEWS AND FEEDBACK

"Dr Drapacz is great and has really helped alleviate many of the problems I have with my feet and ankles. Highly recommended!"
Philip Matuskiewiczv

"Dr Franno and his assistant are extremely professional and super nice. From the moment you check in you feel very welcomed. The office is located in midtown and easy to get too from public transportat…"
Josie J

"Best Place ever to do your feet I did both my feet four years ago , Dr. Fanno and his Staff did a Great Job Love them! Great Staff very Loving ,Supporting and Understanding!"
Marisol Deleon
New York Foot Experts
GET DIRECTIONS
New York Foot Experts
GET DIRECTIONS
*In case of a life-threatening emergency, immediately call 911.
**For any medical procedure, patients respond to treatment differently, hence each patient’s results may vary.
***Information on this site is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. All content contained on or available through this site is for general information purposes only..
****By using this website and sending us your information, you are giving us permission to contact you by electronic and non-electronic means. We also track the conversions and collect user data to improve marketing.
*****If you are vision-impaired or have some other impairment covered by the Americans with Disabilities Act or a similar law, and you wish to discuss potential accommodations related to using this website, please contact us.